
Research in BMM-Lab applies manufacturing science and technology to address clinical unmet needs with three research themes: 1) tissue mechanics and medical imaging, 2) modeling of manufacturing processes, and 3) medical devices and clinical manufacturing systems.
BMM-Lab has currently addressed the following three unmet clinical needs:
-
Plaque narrows arteries and restricts blood flow causing cardiovascular diseases
-
Blood clot blocks arteries and blood flow leading to ischemic stroke
-
Mass customization is needed for personalized medical devices
Plaque narrows arteries

Atherosclerotic plaque is a buildup of calcium, cholesterol, and fat inside the artery wall. The plaque narrows the artery, blocks blood flow, and causes downstream tissue damage. As shown in the figure on the right, plaque in a coronary artery leads to ischemic heart disease—the number one cause of death in the world. The plaque is often calcified and hardened, making it difficult to cut or deform.
To remove calcified plaque, a diamond abrasive grinding wheel rotates at 120,000 – 200,000 rpm inside the artery. It is driven by a long flexible shaft connected to a motor outside the patient’s body. This clinical procedure, called atherectomy, has been used for the past three decades, surprisingly without unanimous guidelines for grinding wheel size and speed selection, and unfortunately with many complications.
To understand the plaque grinding mechanism, we have done the following studies:
Grinding wheel motion and force

Experimental setup for grinding wheel motion and force measurement
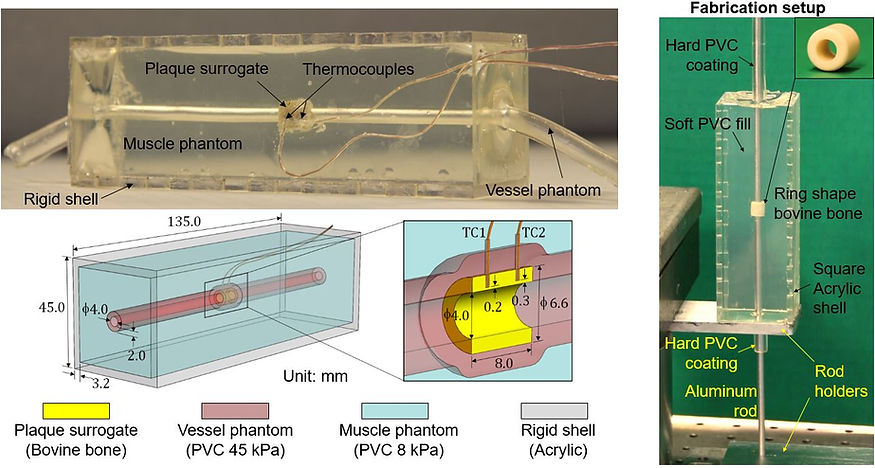
Tissue-mimicking arterial phantom made of bovine bone and soft transparent PVC.
Grinding wheel motion recorded by high-speed camera at 18,000 frames per second.
Wheel rotational speed: 160,000 rpm
Wheel orbital speed: 8,700 rpm
Computational Fluid Dynamics (CFD) Modeling of Wheel Orbital Motion
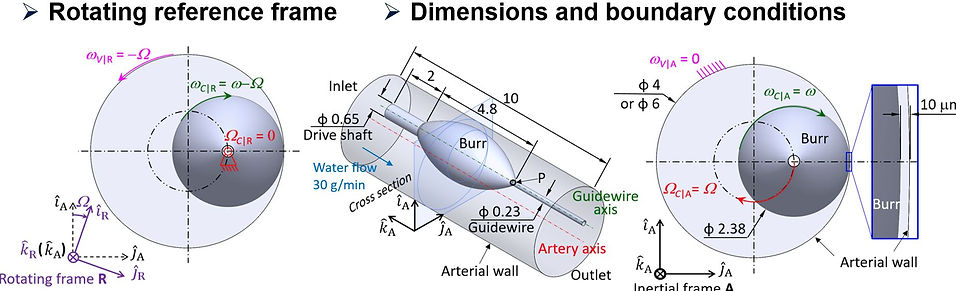

CFD model fomulation with a rotating reference frame to simulate the grinding wheel orbital motion
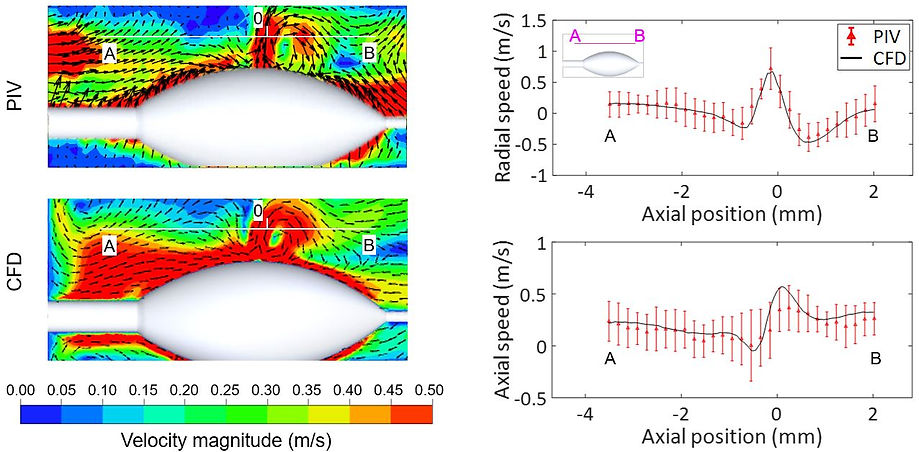
Particle imaging velocimetry (PIV) experimental setup for CFD model validation
Agreement between CFD and PIV results
Smoothed Particle Hydrodynamics (SPH) Modeling of Plaque Grinding

Workpiece modeling with SPH particles coupled with Lagrangian Finite Elements (LEF)

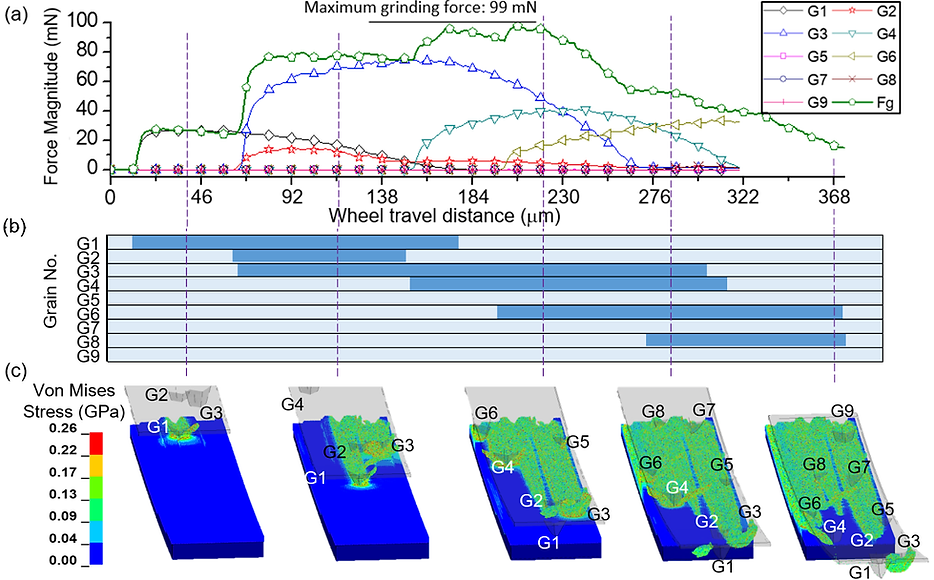
Multi-grain grinding wheel modeling based on confocal measurement of wheel surface topography
SPH multi-grain grinding simulation results
Ultrasound Evaluation of Diseased Vessel Property
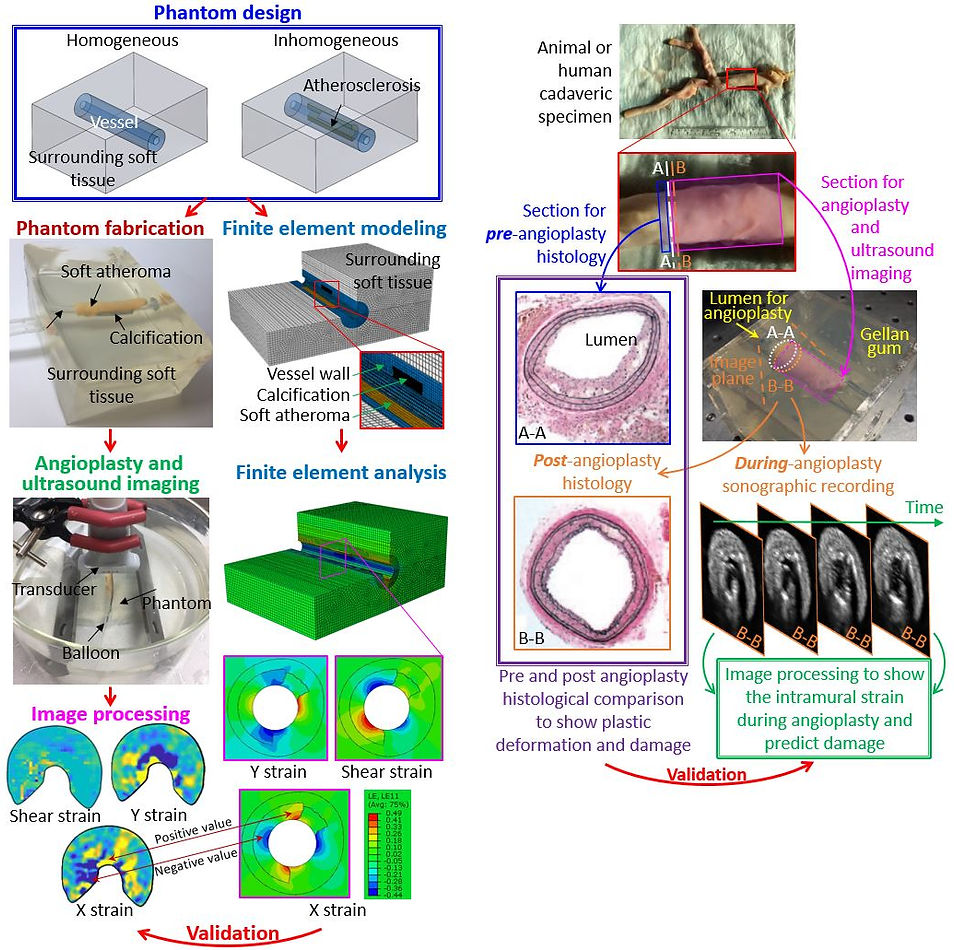
Bench-top and cadaveric tests for validation of ultrasound vascular evaluation algorithm
Blood clot occludes arteries
A blood clot is a gel-like clump of coagulated blood, consisting of a mesh of cross-linked fibrin protein and aggregated platelets and red blood cells. The clot could form inside a vessel or a heart chamber and flow to occlude arteries in the brain, causing a stroke. Stroke is the leading cause of long-term disability in the US.
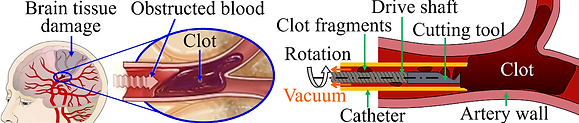
A clot cutting and retrieval (thrombectomy) device has been developed in collaboration with UM Neurosurgery. As illustrated in the figure above, a vacuum catheter passed from the femoral artery to the blocked cerebral artery sucks the clot into the tip. Inside the catheter, a cutting tool driven by a long flexible shaft (inspired by the atherectomy) rotates to fragment the engaged clot near the catheter tip to allow continuous and complete clot removal.
Clot Machining

Experimental setup of blood clot machining and high-speed imaging of clot machining
The blood clot is a difficult-to-machine material. It consists of a mesh of cross-linked fibrin protein and aggregated platelets and red blood cells that form a plug, as shown in the figure on the right. Under loading, the fibrin mesh and surrounding blood cells are stretched/compacted and reoriented, which lead to the nonlinear viscoelasticity of the clot.
We have done the following studies to understand clot tissue mechanics:
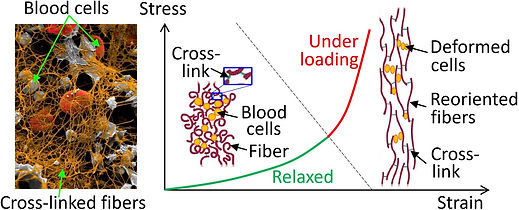
Clot Tissue Mechanics and Cutting Mechanics


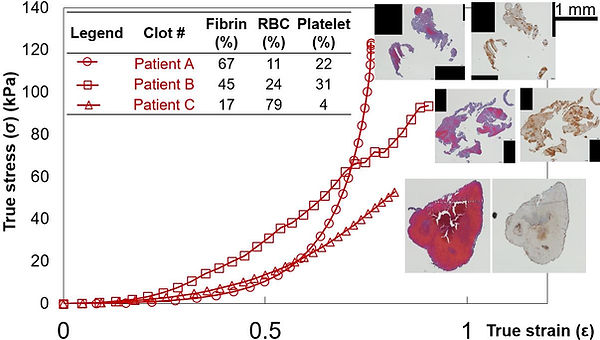
Tensile tests on clots clinically removed from the stroke patients
Histological analysis of patient clots and correlation with tensile properties


Engineered blood clot analog made from human blood products
Blade cutting and needle insertion tests on clot analog
Device Commercialization - Clot Buster
We have developed a mechanical thrombectomy device: Clot Buster for emergency treatment of ischemic stroke caused by large vessel occlusion.

Custom device design and fabrication are challenging
No two patients are alike. Mass customization of personalized assistive devices is commonly needed in healthcare, but the challenges are fit, comfort, and cost. Custom earmold manufacturing for pediatric hearing aids demonstrates these challenges.